Quick Facts: The No Surprises Act (NSA)
| Legal Aspect | Patient Protection Details |
|---|---|
| Emergency Services | Bans out-of-network bills for emergency care, even at out-of-network hospitals. |
| In-Network Facilities | Bans out-of-network charges from providers (e.g., anesthesiologists, radiologists) working at in-network hospitals. |
| Patient Liability | You are only responsible for your standard in-network cost-sharing (co-pay, deductible). |
| Uninsured Patients | Requires a “Good Faith Estimate” upfront. You can dispute bills that exceed the estimate by $400 or more. |
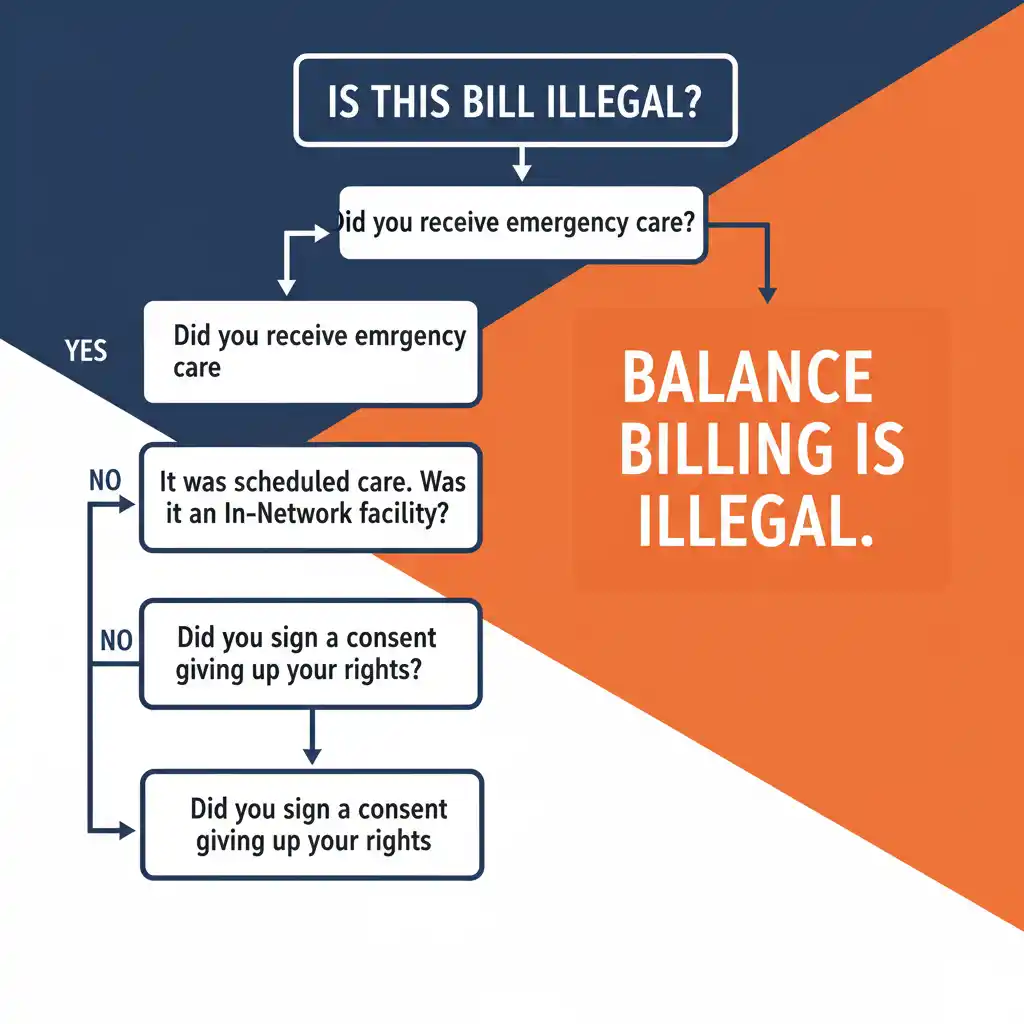
The Trap of “Balance Billing”
For decades, patients played by the rules: they checked their insurance directory, chose an “in-network” hospital for surgery, and assumed they were covered. Weeks later, they would receive a devastating surprise bill for thousands of dollars. Why? Because the anesthesiologist or radiologist who treated them was an independent contractor who did not accept their insurance. The provider would then bill the patient for the difference between their full price and what the insurance paid—a predatory practice known as Balance Billing.
Effective January 1, 2022, the federal No Surprises Act (NSA) made this practice largely illegal. Yet, due to administrative chaos and hospital billing errors, illegal surprise bills are still routinely mailed to patients. You must know how to spot them and invoke your federal rights.
Typical Financial Scenario: The Phantom Anesthesiologist
Presentation: A patient undergoes an emergency appendectomy at an in-network hospital. Their in-network deductible is already met, so they expect no further charges.
The Bill: A month later, an invoice arrives from “Regional Anesthesia Group” for $3,500. The patient’s insurance EOB (Explanation of Benefits) shows they denied the claim because the provider was “Out-of-Network.”
Resolution: The patient recognizes this is a violation of the No Surprises Act. They do not pay the bill. They contact the hospital’s billing department, state that the charge violates the NSA, and demand the bill be withdrawn and settled directly with the insurance company. The balance is reduced to $0.
How to Invoke Your Rights Under the NSA
If you receive a bill that you suspect is an illegal balance bill, follow this immediate action protocol:
1. Do Not Pay the Bill Immediately
Once you pay an illegal bill, getting a refund from an out-of-network provider is incredibly difficult. Put a freeze on the payment while you investigate.
2. Check for the “Notice and Consent” Form
There is a loophole in the law. For non-emergency services, an out-of-network provider can legally balance bill you if and only if they gave you a specific, written “Notice and Consent” document at least 72 hours before the procedure, and you signed it. Note: Certain providers (like anesthesiologists, radiologists, and pathologists) are strictly forbidden from asking you to waive your rights, even for scheduled surgeries.
3. Use the Magic Words with the Billing Department
Call the phone number on the bill. Use this specific script:
“I received this bill for an out-of-network provider at an in-network facility. Under the federal No Surprises Act, I am only responsible for my in-network cost-sharing. I am requesting that you place my account on hold and re-process this claim with my insurance company according to federal law.”
4. File a Federal Complaint
If the provider refuses to drop the charge, do not argue endlessly. File a formal complaint directly with the No Surprises Help Desk (run by the Centers for Medicare & Medicaid Services – CMS). A federal inquiry usually forces the provider to drop the illegal charges immediately.
What if the Insurance Denies the “In-Network” Portion?
Sometimes, the hospital bills correctly, but your insurance company unlawfully denies the claim claiming it wasn’t a “true emergency” or lacking “medical necessity.” If this happens, the No Surprises Act won’t help you, but the standard appeals process will. You must push back.
Use our Free AI Appeal Letter Generator to quickly draft a strong, evidence-based appeal letter to fight a denied claim.
Frequently Asked Questions
Does the No Surprises Act cover urgent care centers?
It depends. The NSA covers emergency services at hospital emergency rooms and freestanding emergency departments. It generally does not cover standard Urgent Care clinics unless the clinic is licensed by the state to provide true emergency services.
What is a Good Faith Estimate for uninsured patients?
If you are uninsured or self-paying, the NSA requires healthcare providers to give you a “Good Faith Estimate” of the total expected costs before you receive care. If your final bill arrives and is $400 or more above that estimate, you have the right to dispute the bill through a federal Patient-Provider Dispute Resolution process.
