Clinical Definition
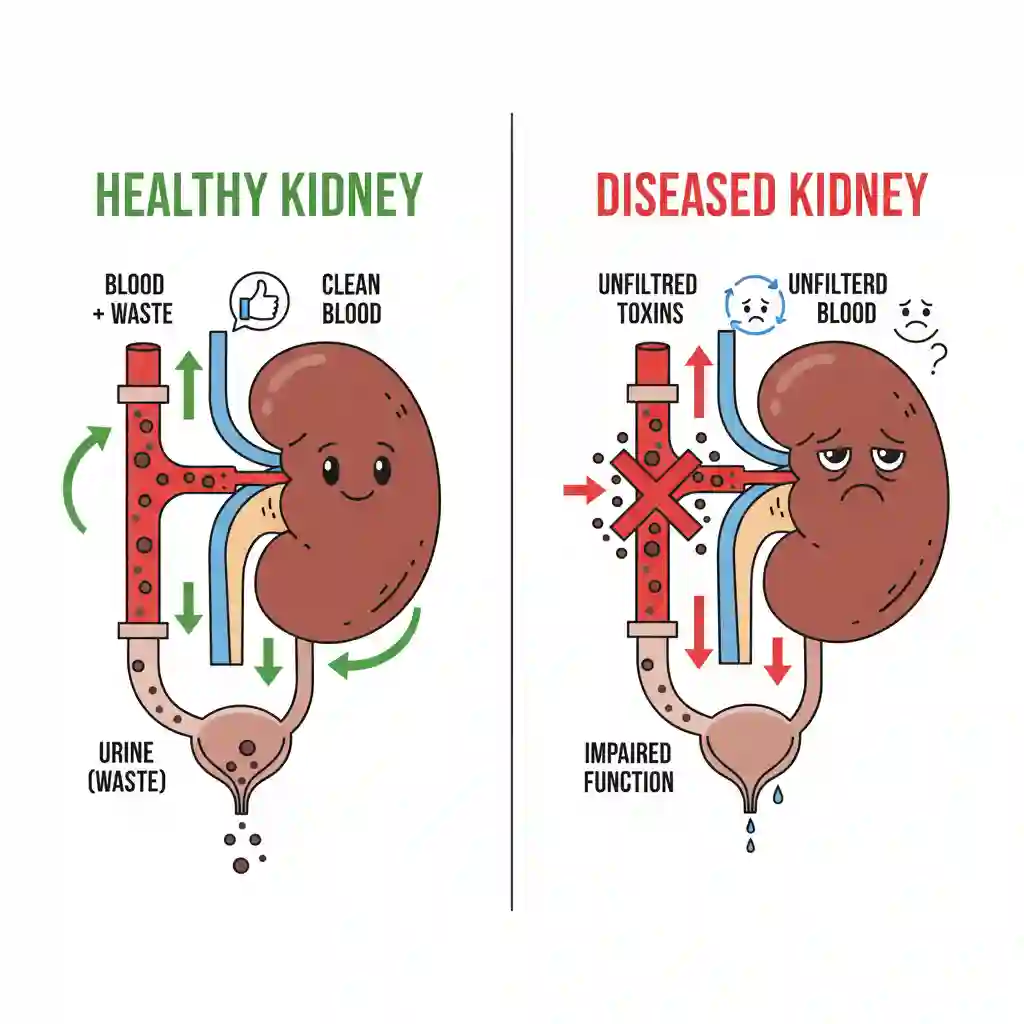
Uremia is the clinical syndrome associated with fluid, electrolyte, and hormone imbalances and metabolic abnormalities, which develop in parallel with the deterioration of renal function. It typically manifests when the Glomerular Filtration Rate (GFR) falls below 10-15 mL/min (End-Stage Renal Disease). The condition is defined by the systemic accumulation of “uremic retention solutes” (toxins) that are normally cleared by healthy kidneys, leading to multi-organ dysfunction.
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | N18.6 | End stage renal disease (ESRD) |
| ICD-10-CM | N19 | Unspecified kidney failure (includes Uremia NOS) |
| CPT (Procedural) | 90935 – 90937 | Hemodialysis procedure with single physician evaluation |
| CPT (Procedural) | 90945 | Dialysis procedure other than hemodialysis (e.g., Peritoneal) |
| Affected System | Renal; Metabolic; Cardiovascular | Systemic toxicity due to renal failure |
Epidemiology & Statistics
End-Stage Renal Disease (ESRD) represents a significant global public health burden. In the United States, data from the United States Renal Data System (USRDS) indicates that the prevalence of ESRD continues to rise, driven largely by aging populations and the increasing incidence of metabolic syndrome. The two primary etiologies accounting for over 70% of incident cases are Diabetes Mellitus (Diabetic Nephropathy) and Hypertension (Hypertensive Nephrosclerosis). Other contributing factors include Glomerulonephritis and Polycystic Kidney Disease.
Pathophysiology (Mechanism)
The pathophysiology of uremia is characterized by the retention of uremic solutes due to the loss of nephron mass. Mechanistically, this involves:
1. Accumulation of Organic Waste: Nitrogenous waste products (Urea, Creatinine) and “middle molecules” (e.g., Beta-2 microglobulin) accumulate in the serum, exerting toxic effects on cellular functions.
2. Electrolyte and Acid-Base Dysregulation: The failing kidney loses the ability to excrete potassium (leading to Hyperkalemia) and hydrogen ions (leading to Metabolic Acidosis), disrupting cellular membrane potentials and enzymatic function.
3. Endocrine Dysfunction:
– Reduced production of Erythropoietin (EPO) leads to normocytic, normochromic anemia.
– Impaired hydroxylation of Vitamin D results in hypocalcemia and secondary hyperparathyroidism (Renal Osteodystrophy).
Standard Management Protocols
Management of uremia requires Renal Replacement Therapy (RRT) alongside pharmacological management of comorbidities.
- Pharmacological Classes:
- Erythropoiesis-Stimulating Agents (ESAs): Recombinant analogs of erythropoietin used to stimulate red blood cell production in the bone marrow to manage anemia of chronic disease.
- Phosphate Binders: Polymers or salts (e.g., Calcium acetate, Sevelamer) that bind dietary phosphorus in the gastrointestinal tract to prevent absorption and manage hyperphosphatemia.
- Calcimimetics: Agents that increase the sensitivity of the calcium-sensing receptor on the parathyroid gland to suppress Parathyroid Hormone (PTH) secretion.
- Surgical/Procedural Interventions (RRT):
- Hemodialysis (HD): Extracorporeal removal of waste products and free water via an artificial semipermeable membrane. Requires vascular access (AV Fistula or Graft).
- Peritoneal Dialysis (PD): Uses the patient’s peritoneal membrane as a filter. Dialysate is dwelled in the abdominal cavity to facilitate exchange via osmosis and diffusion.
- Renal Transplantation: The definitive treatment for eligible candidates, restoring renal function via allograft.
Healthcare Resource Utilization
Uremia management is associated with extremely high healthcare resource utilization. Key factors include:
- Vascular Access Maintenance: Frequent surgical interventions are often required to maintain patency of Arteriovenous (AV) Fistulas or Grafts.
- Chronic Logistics: Hemodialysis typically requires attendance at a specialized center three times weekly for 3-4 hours per session.
- Hospitalization Rates: Patients with uremia have higher rates of hospitalization due to cardiovascular events and infections compared to the general population.