Clinical Definition
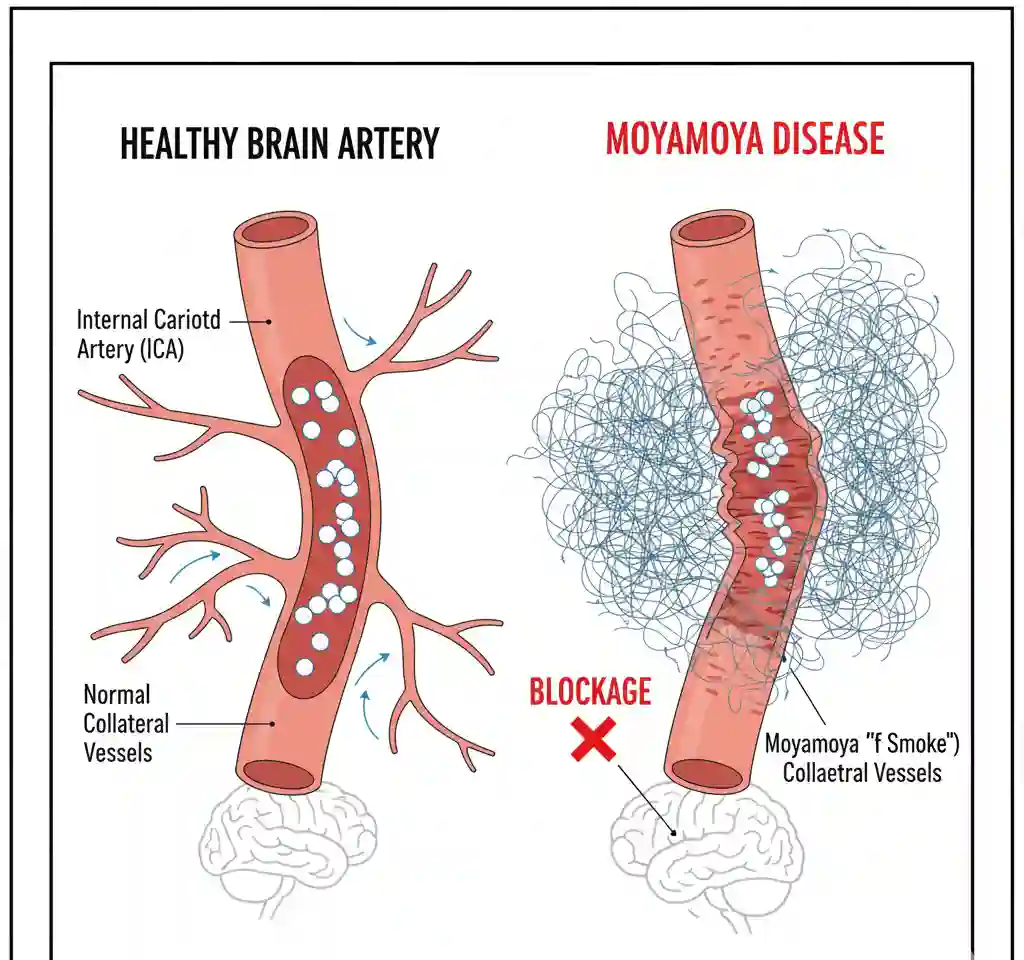
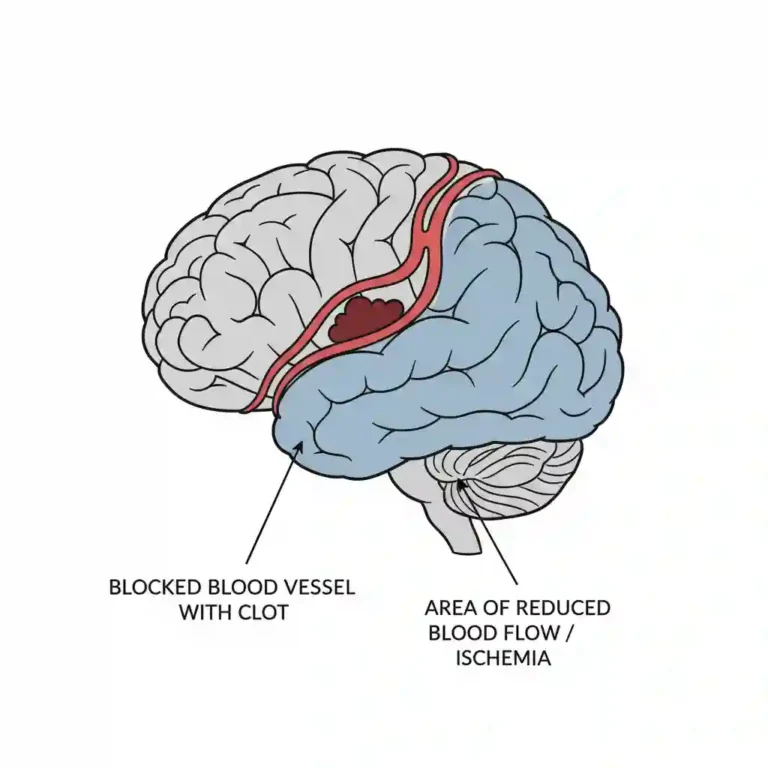
Moyamoya disease (MMD) is a rare, progressive chronic cerebrovascular occlusive disease characterized by bilateral steno-occlusive changes at the terminal portion of the internal carotid artery and the proximal portions of the anterior and middle cerebral arteries. The condition is distinctively marked by the development of an abnormal vascular network (collateral circulation) at the base of the brain, referred to as “moyamoya” vessels. This vascular instability frequently results in cerebral hypoperfusion, leading to ischemic or hemorrhagic cerebrovascular events.
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | I67.5 | Moyamoya disease |
| ICD-10-CM | I67.89 | Other specified cerebrovascular diseases (often used for Moyamoya syndrome) |
| CPT (Diagnostic) | 36224 | Selective catheter placement, internal carotid artery, unilateral, with angiography |
| CPT (Surgical) | 61711 | Anastomosis, arterial, extracranial-intracranial (e.g., middle cerebral/superficial temporal) |
| Affected System | N/A | Cerebrovascular System; Central Nervous System |
Epidemiology & Statistics
Epidemiological data indicates a marked ethnic predisposition, with the highest prevalence observed in East Asian populations, particularly in Japan, Korea, and China. The disease exhibits a bimodal age distribution, with a pediatric peak occurring between 5 and 10 years of age, and a second adult peak between 30 and 40 years. There is a noted female predominance, with a female-to-male ratio approximating 2:1. While familial occurrence accounts for approximately 10-15% of cases, suggesting a genetic etiology (e.g., RNF213 gene mutation), the majority of cases are sporadic.
Pathophysiology (Mechanism)
The primary pathological feature is the fibrocellular intimal thickening of the arterial walls, specifically involving the terminal internal carotid arteries. This is driven by the proliferation of smooth muscle cells, which leads to progressive luminal stenosis and eventual occlusion.
In response to this reduced cerebral perfusion pressure (CPP), the brain recruits compensatory mechanisms: the dilation of perforating arteries and the development of fragile collateral vessels (moyamoya vessels) at the base of the brain. These collaterals are structurally weak and prone to rupture (microaneurysm formation), leading to the hemorrhagic presentation common in adults. Conversely, the stenosis itself causes hypoperfusion, resulting in the ischemic presentation (TIAs and infarction) more commonly observed in pediatric cohorts.
Standard Management Protocols
Management strategies are stratified based on symptomatic presentation (ischemic vs. hemorrhagic) and hemodynamic reserve status.
- Pharmacological Classes:
- Antiplatelet Agents: Agents such as Acetylsalicylic acid (Aspirin) are frequently employed in ischemic presentations to inhibit cyclooxygenase (COX) activity and reduce platelet aggregation, thereby minimizing thrombotic risk in stenotic vessels.
- Calcium Channel Blockers: May be utilized to manage associated headaches or migraines, though their use requires careful titration to avoid hypotension-induced hypoperfusion.
- Anticonvulsants: Indicated for seizure management secondary to cortical ischemia or hemorrhage.
- Surgical/Procedural Interventions (Revascularization):
- Direct Bypass: Superficial Temporal Artery to Middle Cerebral Artery (STA-MCA) anastomosis. Provides immediate flow augmentation.
- Indirect Bypass: Encephalo-duro-arterio-synangiosis (EDAS) or Encephalo-myo-synangiosis (EMS). Relies on angiogenesis from vascularized donor tissues (scalp, muscle, dura) onto the cortical surface.
- Combined Revascularization: Utilizing both direct and indirect techniques to maximize collateral development.
Healthcare Resource Utilization
Moyamoya disease imposes a significant burden on healthcare resources due to the requirement for lifelong surveillance. Economic factors include:
- Diagnostic Imaging Burden: Repeated high-resolution imaging (MRI, MRA, Digital Subtraction Angiography, and Perfusion CT/MRI) is required for preoperative assessment and postoperative follow-up to monitor graft patency and disease progression.
- Surgical Complexity: Revascularization procedures require specialized neurosurgical facilities and often necessitate ICU admission for strict blood pressure management post-operatively to prevent hyperperfusion syndrome.
- Rehabilitation: Patients sustaining cerebrovascular accidents (stroke) may require extensive physical, occupational, and speech therapy services.