Executive Summary
Glucose metabolism is a core physiological process essential for maintaining systemic energy supply. The process involves the digestion of carbohydrates into glucose, its absorption into the bloodstream, and its subsequent hormonal regulation to ensure a stable supply of energy for all cellular functions, particularly for the central nervous system. The endocrine pancreas, through the coordinated secretion of insulin and glucagon, is the primary regulator of this homeostatic system, directing the flux of glucose into pathways for immediate energy use (glycolysis), short-term storage (glycogenesis), or long-term storage (lipogenesis).
Key Data Points
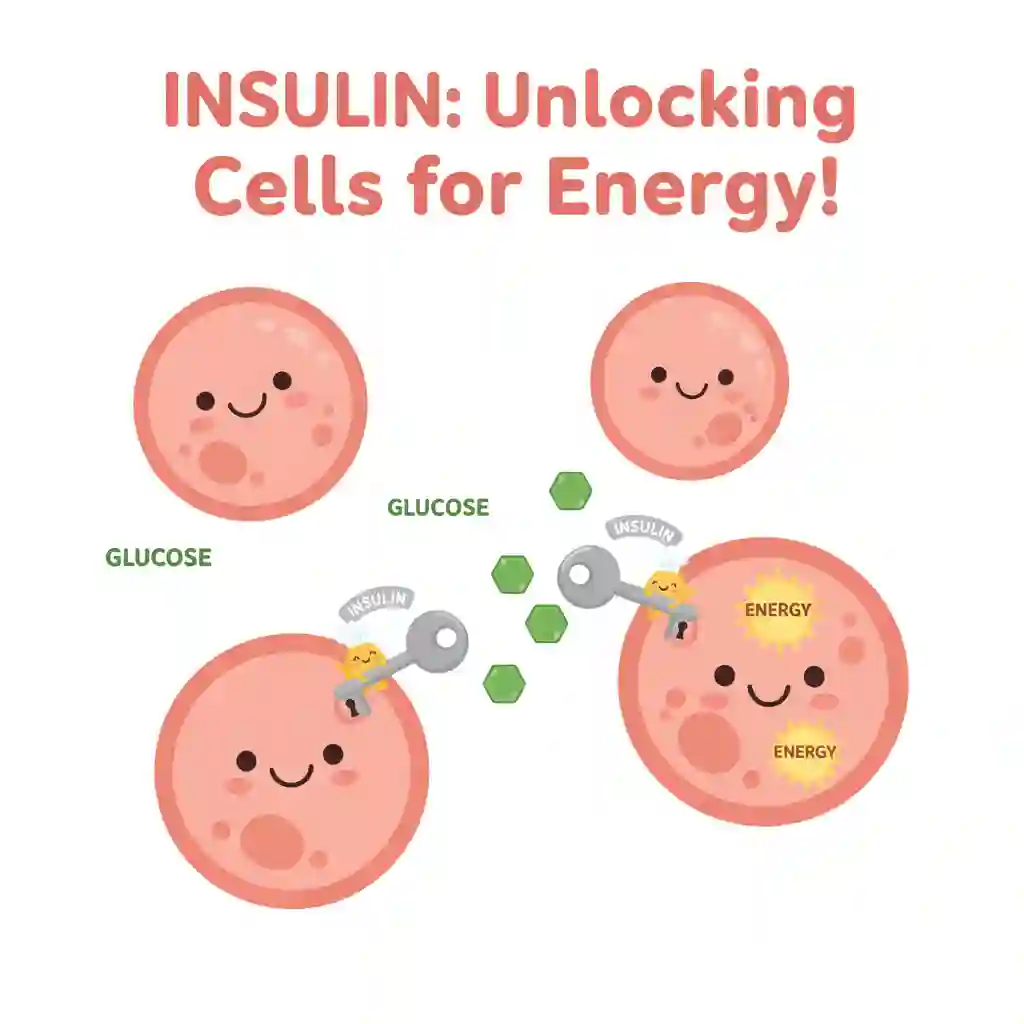
- Postprandial Hyperglycemia & Insulin Response: Following carbohydrate ingestion, rising blood glucose levels stimulate pancreatic beta-cells to secrete insulin. Insulin facilitates the transport of glucose into peripheral cells (e.g., muscle, adipose tissue) for energy production.
- Energy Production (ATP): Intracellularly, glucose is catabolized through glycolysis and the citric acid cycle to produce adenosine triphosphate (ATP), the primary energy currency of the cell.
- Glycogenesis (Short-Term Storage): Excess glucose is polymerized into glycogen and stored in the liver and skeletal muscles under the influence of insulin. Hepatic glycogen is the primary source for maintaining blood glucose during fasting.
- Hypoglycemia & Glucagon Response: In a fasting state, declining blood glucose levels trigger pancreatic alpha-cells to release glucagon.
- Glycogenolysis (Energy Release): Glucagon acts primarily on the liver to stimulate the breakdown of stored glycogen into glucose (glycogenolysis), which is then released into the bloodstream to prevent hypoglycemia.
- Lipogenesis (Long-Term Storage): When glycogen stores are saturated, excess glucose is converted into fatty acids and stored as triglycerides in adipose tissue.
Research Methodology / Context
The principles of glucose homeostasis are foundational concepts in biochemistry and endocrinology, established through decades of research. Methodologies used to study these pathways include oral glucose tolerance tests (OGTT) to assess insulin response, radioimmunoassays to measure circulating hormone levels (insulin, glucagon, cortisol), and isotope tracer studies to track the metabolic fate of glucose molecules in vivo. The scientific context is the body’s intricate system of feedback loops designed to maintain metabolic equilibrium in the face of fluctuating dietary intake and energy expenditure.
Clinical Implications
- Foundation of Metabolic Disease: Dysregulation of this system is the pathophysiological basis for metabolic disorders, most notably Diabetes Mellitus (Type 1 involving insulin deficiency; Type 2 involving insulin resistance).
- Diagnostic Markers: Clinical assessment of glucose homeostasis through measurements of fasting plasma glucose, HbA1c, and OGTT results are the standard diagnostic criteria for prediabetes and diabetes.
- Therapeutic Targets: The majority of antidiabetic pharmacotherapies are designed to target specific points in this pathway, such as enhancing insulin secretion, improving insulin sensitivity, or reducing hepatic glucose production.
- Basis for Non-Pharmacological Interventions: Lifestyle interventions, including dietary modifications (e.g., managing carbohydrate intake) and physical exercise (which improves insulin sensitivity), are effective because they directly modulate the key pathways of glucose metabolism.