Coronary Angiography: Diagnostic Protocol & Technical Specifications
Procedure Overview & Indications
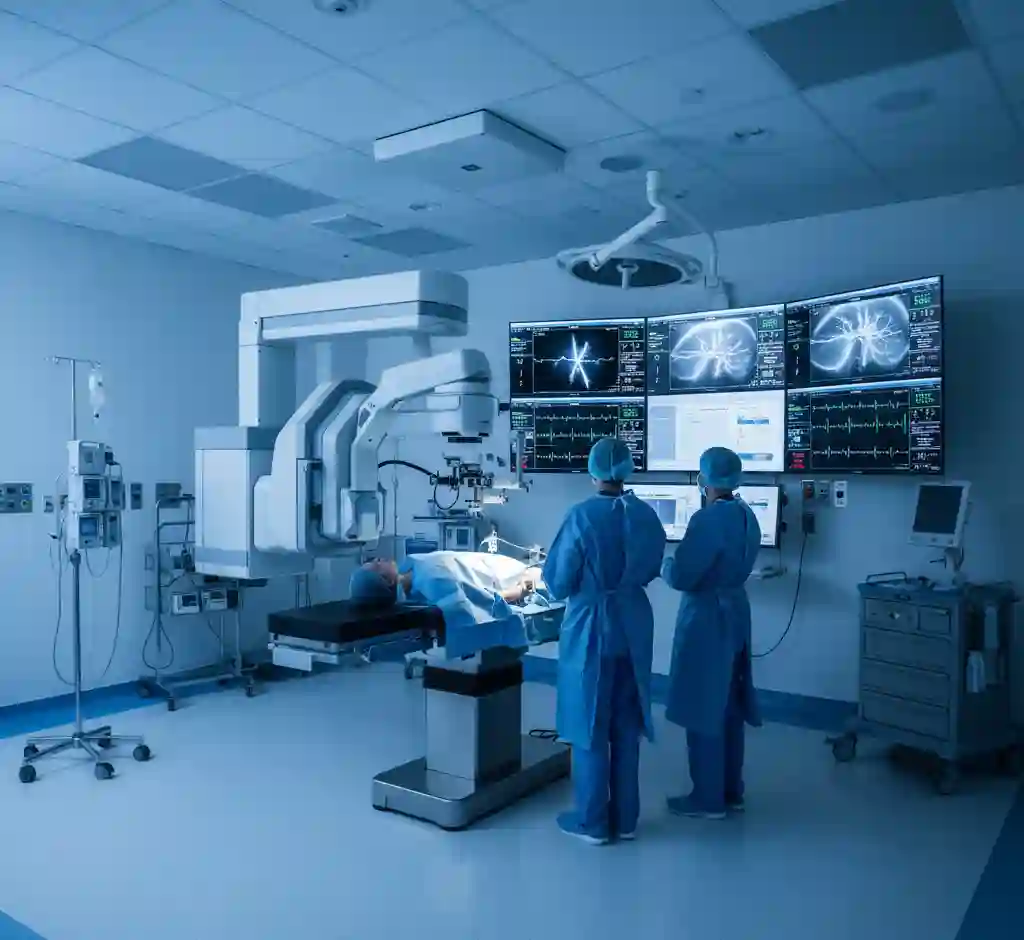
Coronary Angiography (Cardiac Catheterization) is an invasive diagnostic imaging procedure that utilizes radiopaque contrast media and fluoroscopic X-ray technology to visualize the lumen of the coronary arteries and cardiac chambers. It remains the gold standard for the anatomical assessment of Coronary Artery Disease (CAD).
Primary Indications:
- Evaluation of ST-Elevation Myocardial Infarction (STEMI) and NSTEMI.
- Assessment of stable angina unresponsive to medical therapy.
- Pre-operative assessment prior to valvular surgery or Congenital Heart Disease (CHD) repair.
- Post-intervention surveillance of stent patency.
Procedural Coding & Billing
Accurate coding depends on the access site, vessels visualized, and concurrent interventions.
- CPT Code Range (Diagnostic):
- 93454: Catheter placement in coronary artery(s) for coronary angiography.
- 93458: With left heart catheterization (LHC) including intra-procedural ventricular/atrial angiography.
- 93503: Insertion and placement of flow directed catheter (Swan-Ganz) for monitoring.
- ICD-10-PCS (Inpatient Procedure Coding):
- 4A023N7: Measurement of Cardiac Sampling and Pressure, Left Heart, Percutaneous Approach.
- B2111ZZ: Fluoroscopy of Multiple Coronary Arteries using Low Osmolar Contrast.
Technology & Equipment
The procedure requires a specialized Cardiac Catheterization Laboratory (“Cath Lab”) equipped with high-resolution imaging and hemodynamic monitoring systems.
- Imaging System: C-Arm Fluoroscopy unit (e.g., Philips Allura, Siemens Artis) capable of rotational angiography and digital subtraction angiography (DSA).
- Vascular Access:
- Introducer Sheaths (5F or 6F) with hemostatic valves.
- Diagnostic Catheters: Judkins Left (JL), Judkins Right (JR), and Pigtail catheters for ventriculography.
- Contrast Media: Non-ionic, low-osmolar or iso-osmolar iodinated contrast agents (e.g., Iodixanol) to minimize renal toxicity (CIN).
- Hemodynamic Monitoring: Polygraph system for real-time recording of aortic and ventricular pressures.
Methodology (Step-by-Step Summary)
The procedure follows the Seldinger technique for vascular access, typically via the radial or femoral artery.
1. Preparation Phase
Patient is positioned supine on the radiolucent table. Sterile draping is applied. Local anesthetic (1-2% Lidocaine) is infiltrated at the access site. Continuous ECG and pulse oximetry monitoring are established.
2. Procedural Phase
- Arterial Access: Puncture of the radial (preferred) or femoral artery. Insertion of a hydrophilic guidewire followed by the introducer sheath.
- Catheter Navigation: Under fluoroscopic guidance, the diagnostic catheter is advanced over a guidewire up the aorta to the coronary ostia.
- Contrast Injection: The guidewire is removed, and the catheter is engaged in the coronary ostium. Contrast media (approx. 4-8ml per injection) is injected manually or via an automated power injector.
- Cine-Angiography: X-ray footage is recorded in multiple orthogonal views (RAO/LAO projections with Cranial/Caudal angulation) to minimize vessel overlap and foreshortening.
3. Post-Procedural Monitoring
Sheath removal is performed with mechanical compression devices (e.g., TR Band for radial access) or vascular closure devices (e.g., Angio-Seal). Activated Clotting Time (ACT) is monitored if heparin was administered.
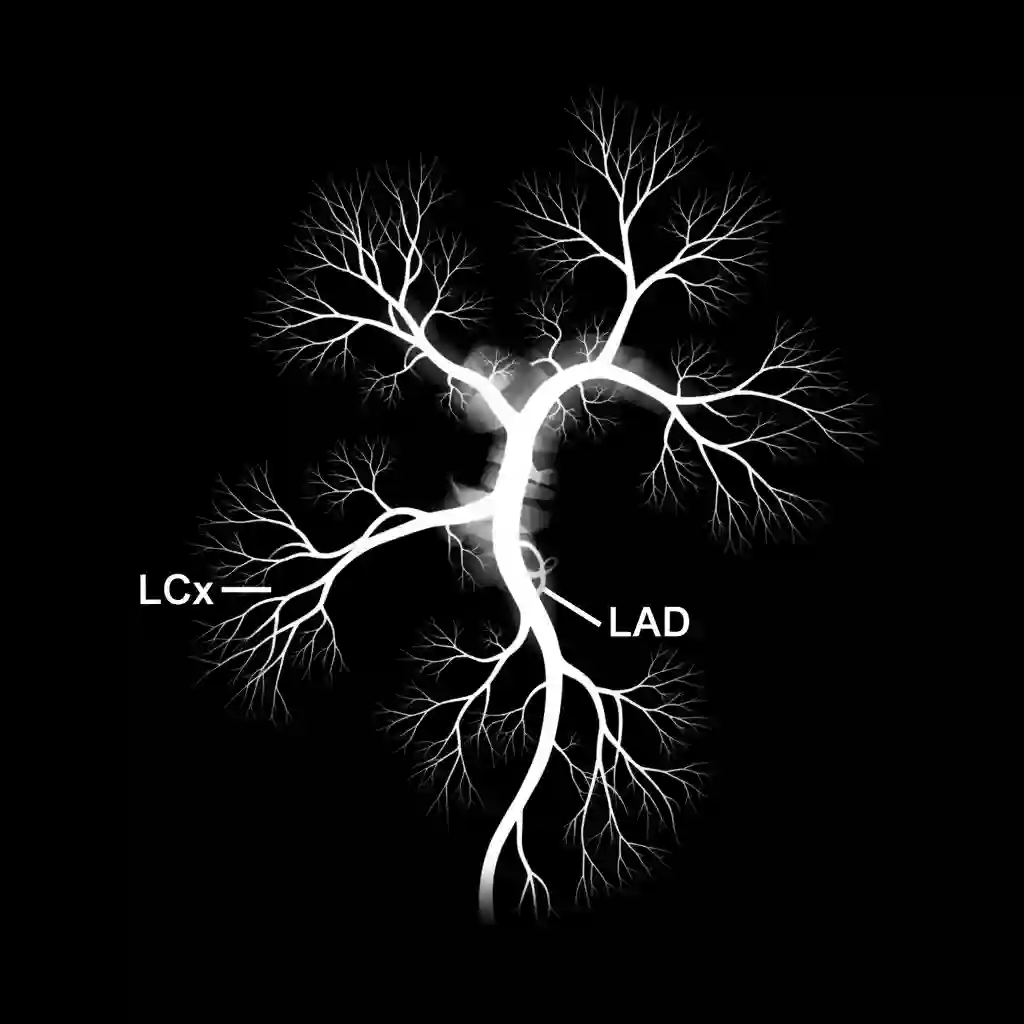
Clinical Significance & Outcomes
The angiographic data allows for the calculation of quantitative stenosis severity.
- Significant Stenosis: Typically defined as ≥70% reduction in luminal diameter (≥50% for the Left Main artery).
- TIMI Flow Grade: Used to assess coronary blood flow (Grade 0 = No perfusion; Grade 3 = Complete perfusion).
- Fractional Flow Reserve (FFR): If anatomical severity is ambiguous, a pressure wire may be used to measure the physiological significance of the lesion (FFR ≤ 0.80 indicates ischemia).