Clinical Definition
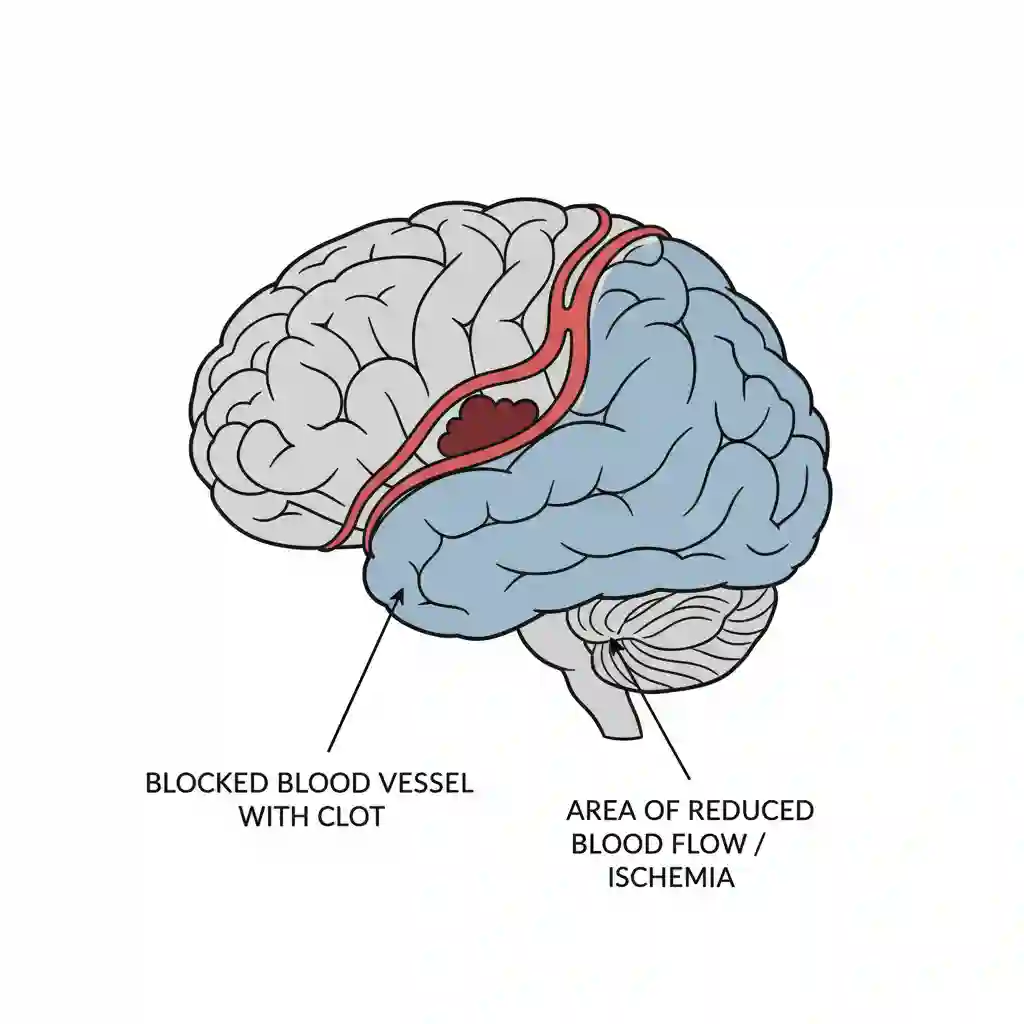
Cerebral infarction, clinically termed ischemic stroke, is defined as an episode of neurological dysfunction caused by focal cerebral, spinal, or retinal infarction. It is characterized by the irreversible necrosis of brain tissue resulting from a critical reduction in cerebral blood flow (CBF) due to arterial occlusion (thrombosis or embolism). Diagnosis requires objective evidence of infarction on neuroimaging (MRI-DWI or CT) or clinical persistence of symptoms for ≥24 hours.
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | I63.9 | Cerebral infarction, unspecified |
| ICD-10-CM | I63.0 – I63.5 | Cerebral infarction due to thrombosis/embolism of specific arteries (Precerebral/Cerebral) |
| CPT (Therapeutic) | 37184 | Primary percutaneous transluminal mechanical thrombectomy (intracranial) |
| CPT (Therapeutic) | 37211 | Intracranial thrombolysis (infusion) |
| DRG (Inpatient) | 061 – 063 | Ischemic Stroke, Precerebral Occlusion, or TIA |
Epidemiology & Statistics
Ischemic stroke accounts for approximately 87% of all stroke cases globally. It remains a leading cause of long-term adult disability and is the fifth leading cause of death in the United States. Etiological classification typically follows the TOAST criteria: Large Artery Atherosclerosis (~20%), Cardioembolism (~25%), Small Vessel Occlusion (Lacunar, ~25%), and Cryptogenic/Other (~30%). Incidence increases significantly with age, and key modifiable risk factors include hypertension, atrial fibrillation, diabetes mellitus, and dyslipidemia.
Pathophysiology (Mechanism)
The core mechanism involves the Ischemic Cascade. Following arterial occlusion:
1. Energy Failure: Lack of oxygen and glucose leads to ATP depletion, causing failure of the Na+/K+ ATPase pump.
2. Excitotoxicity: Membrane depolarization triggers an excessive release of glutamate, leading to massive calcium influx via NMDA receptors.
3. Cell Death: Intracellular calcium overload activates proteases and lipases, destroying cell structures (necrosis).
4. Penumbra Concept: Clinically, the brain tissue is divided into the “Ischemic Core” (irreversible damage) and the “Penumbra” (hypoperfused but salvageable tissue). Reperfusion therapies aim to salvage the penumbra before it progresses to infarction.
Standard Management Protocols
Acute management focuses on rapid restoration of cerebral perfusion (reperfusion strategies).
- Pharmacological Classes:
- Thrombolytics (Fibrinolytics): (e.g., Alteplase, Tenecteplase) These agents activate plasminogen to form plasmin, which degrades fibrin clots. Indicated within a specific time window (usually <4.5 hours) from symptom onset.
- Antiplatelet Agents: (e.g., Aspirin, Clopidogrel) Inhibits platelet aggregation (via COX-1 or P2Y12 inhibition) for secondary prevention.
- Anticoagulants: (e.g., Warfarin, DOACs) Indicated for cardioembolic etiology (e.g., Atrial Fibrillation).
- Surgical/Procedural Interventions:
- Mechanical Thrombectomy (EVT): Endovascular removal of the thrombus using stent retrievers or aspiration catheters. Standard of care for Large Vessel Occlusion (LVO) in the anterior circulation.
- Carotid Endarterectomy (CEA): Surgical removal of plaque from the carotid artery for significant stenosis.
Healthcare Resource Utilization
Cerebral infarction management is resource-intensive, involving:
- Emergency Infrastructure: Utilization of “Stroke Code” protocols, CT/CTA imaging prioritization, and Tele-stroke networks.
- Critical Care: Many patients require Neuro-ICU admission for blood pressure management and monitoring for cerebral edema.
- Long-term Rehabilitation: Significant expenditure on physical, occupational, and speech therapy for functional recovery.