Clinical Definition
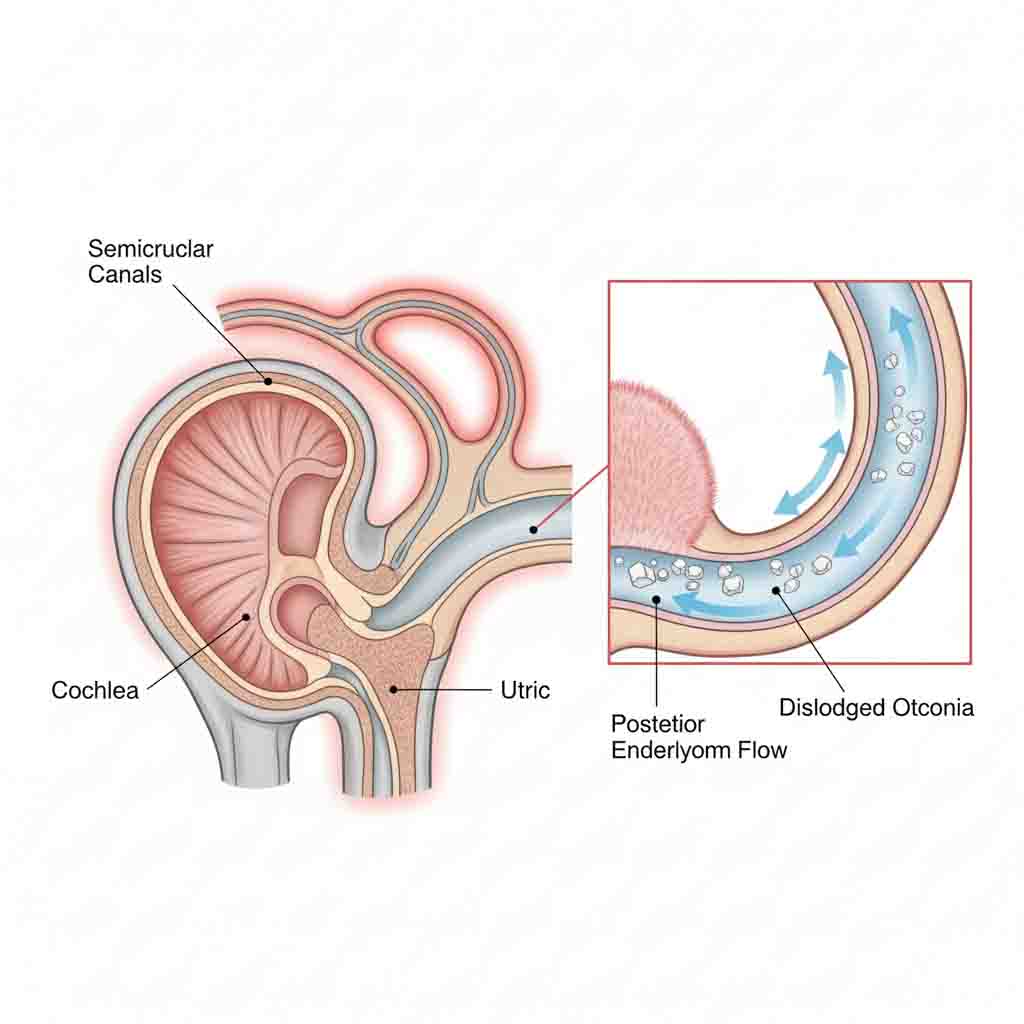
Benign Paroxysmal Positional Vertigo (BPPV) is a mechanical disorder of the peripheral vestibular system. It is characterized by brief, intense episodes of vertigo triggered by specific changes in the position of the head relative to gravity. The condition arises from otolithiasis, where calcium carbonate crystals (otoconia), normally embedded in the utricular macula, become dislodged and migrate into the semicircular canals (canalithiasis) or adhere to the cupula (cupulolithiasis), disrupting normal endolymphatic fluid dynamics.
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | H81.1 | Benign paroxysmal vertigo |
| ICD-10-CM | H81.11 / H81.12 | Benign paroxysmal vertigo, right ear / left ear |
| CPT (Therapeutic) | 95992 | Canalith repositioning procedure(s) (e.g., Epley maneuver), including neurological exam |
| CPT (Diagnostic) | 92538 | Caloric vestibular testing |
| Affected System | Vestibular; Neurological | Posterior Semicircular Canal (most common) |
Epidemiology & Statistics
BPPV is the most common cause of peripheral vertigo, accounting for approximately 17% to 42% of patients presenting with dizziness. The lifetime prevalence is estimated at 2.4%. Incidence increases linearly with age, peaking in the 5th to 7th decades of life, likely due to age-related degeneration of the otoliths. There is a female preponderance, with a female-to-male ratio of approximately 2:1.
Pathophysiology (Mechanism)
The clinical presentation depends on the location and behavior of the displaced otoconia:
1. Canalithiasis (Common): Free-floating otoconia in the long arm of the semicircular canal move under gravity during head position changes. This movement creates a hydrodynamic drag on the endolymph, deflecting the cupula and causing nystagmus with a characteristic latency and fatigue.
2. Cupulolithiasis (Rare): Otoconia adhere directly to the cupula, increasing its density and making it gravity-sensitive. This results in immediate, persistent nystagmus without fatigue.
3. Canal Involvement: The Posterior Canal is involved in >85% of cases due to its gravity-dependent position when supine. The Horizontal (Lateral) Canal is involved in ~10-15% of cases.
Standard Management Protocols
Management is primarily mechanical, aiming to return otoconia to the utricle.
- Diagnostic Maneuvers:
- Dix-Hallpike Test: The gold standard for diagnosing Posterior Canal BPPV.
- Supine Roll Test: Used to diagnose Horizontal Canal BPPV.
- Therapeutic Procedures (Canalith Repositioning):
- Epley Maneuver: Standard repositioning procedure for Posterior Canal Canalithiasis.
- Semont Maneuver: An alternative liberatory maneuver for Posterior Canal BPPV.
- Lempert (BBQ) Roll: Used for Horizontal Canal BPPV.
- Pharmacological Classes:
- Vestibular Suppressants: (e.g., Meclizine, Benzodiazepines) Generally contraindicated for chronic use as they do not treat the underlying mechanical problem and may delay central vestibular compensation, but may be used short-term for severe nausea.
Healthcare Resource Utilization
BPPV represents a significant economic burden due to misdiagnosis and high utilization of unnecessary diagnostics:
- Imaging Overuse: A high percentage of patients undergo unnecessary MRI or CT scans before receiving a simple Dix-Hallpike test.
- Fall Risk: In elderly populations, untreated BPPV is a major risk factor for falls and subsequent fractures.