Clinical Definition
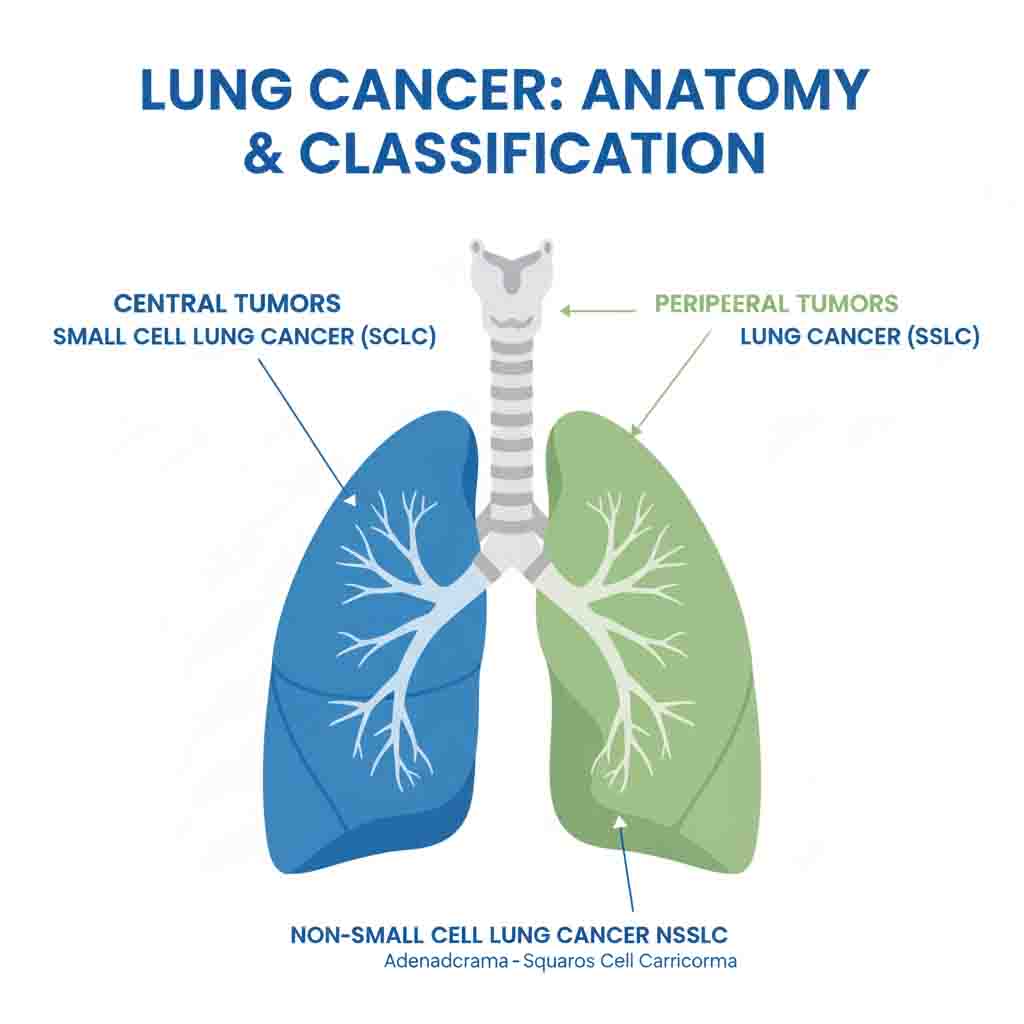
Lung Cancer, or Bronchogenic Carcinoma, is a malignant neoplasm arising from the respiratory epithelium (bronchi, bronchioles, and alveoli). It is histologically categorized into two major classes with distinct clinical behaviors and management protocols: Non-Small Cell Lung Cancer (NSCLC) (approx. 85% of cases, including Adenocarcinoma, Squamous Cell Carcinoma, and Large Cell Carcinoma) and Small Cell Lung Cancer (SCLC) (approx. 15% of cases, characterized by neuroendocrine differentiation, rapid doubling time, and early metastasis).
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | C34.90 | Malignant neoplasm of unspecified part of unspecified bronchus or lung |
| ICD-10-CM | C34.1 | Malignant neoplasm of upper lobe, bronchus or lung |
| CPT (Diagnostic) | 31622 | Bronchoscopy, rigid or flexible, diagnostic |
| CPT (Screening) | 71271 | Computed tomography, thorax, low dose for lung cancer screening (LDCT) |
| Pathology | 81404 | Molecular pathology procedure (e.g., EGFR, KRAS, ALK testing) |
Epidemiology & Statistics
Lung cancer is the leading cause of cancer-related mortality globally. Tobacco smoking is the primary risk factor, implicated in 80-90% of cases. However, the incidence of Adenocarcinoma in non-smokers (particularly women) is rising. NSCLC is typically diagnosed at advanced stages (Stage III/IV), though the implementation of Low-Dose CT (LDCT) screening in high-risk populations aims to improve early detection rates.
Pathophysiology (Mechanism)
Carcinogenesis involves the accumulation of somatic driver mutations:
1. Driver Mutations (NSCLC): Specific genetic alterations drive tumor growth, including EGFR mutations, ALK translocations, ROS1 rearrangements, and KRAS mutations. These are critical targets for precision medicine.
2. Neuroendocrine Differentiation (SCLC): SCLC cells exhibit neuroendocrine markers (e.g., Chromogranin, Synaptophysin) and are often associated with paraneoplastic syndromes (e.g., SIADH, Lambert-Eaton Myasthenic Syndrome).
3. Immune Evasion: Tumors may express PD-L1 (Programmed Death-Ligand 1), which binds to PD-1 on T-cells to inhibit the anti-tumor immune response.
Standard Management Protocols
Management is strictly dictated by Histology (NSCLC vs. SCLC), TNM Stage, and Molecular Profiling.
- Pharmacological Classes (Precision Oncology):
- Tyrosine Kinase Inhibitors (TKIs): (e.g., Osimertinib, Alectinib) Standard of care for EGFR-mutant or ALK-positive NSCLC.
- Immune Checkpoint Inhibitors (ICI): (e.g., Pembrolizumab, Nivolumab) Monoclonal antibodies targeting PD-1/PD-L1. Used in both NSCLC and extensive-stage SCLC.
- Platinum-Doublet Chemotherapy: (e.g., Cisplatin + Pemetrexed) Traditional cytotoxic therapy.
- Surgical/Procedural Interventions:
- Lobectomy/VATS: Video-Assisted Thoracoscopic Surgery for early-stage resectable NSCLC.
- Stereotactic Body Radiation Therapy (SBRT): For early-stage patients who are medically inoperable.
Healthcare Resource Utilization
Lung cancer care is resource-intensive due to:
- High Drug Costs: Immunotherapy and Targeted Therapies are among the highest-cost pharmaceuticals.
- Diagnostic Complexity: Routine use of PET-CT for staging and Next-Generation Sequencing (NGS) for biomarker testing.