Clinical Definition
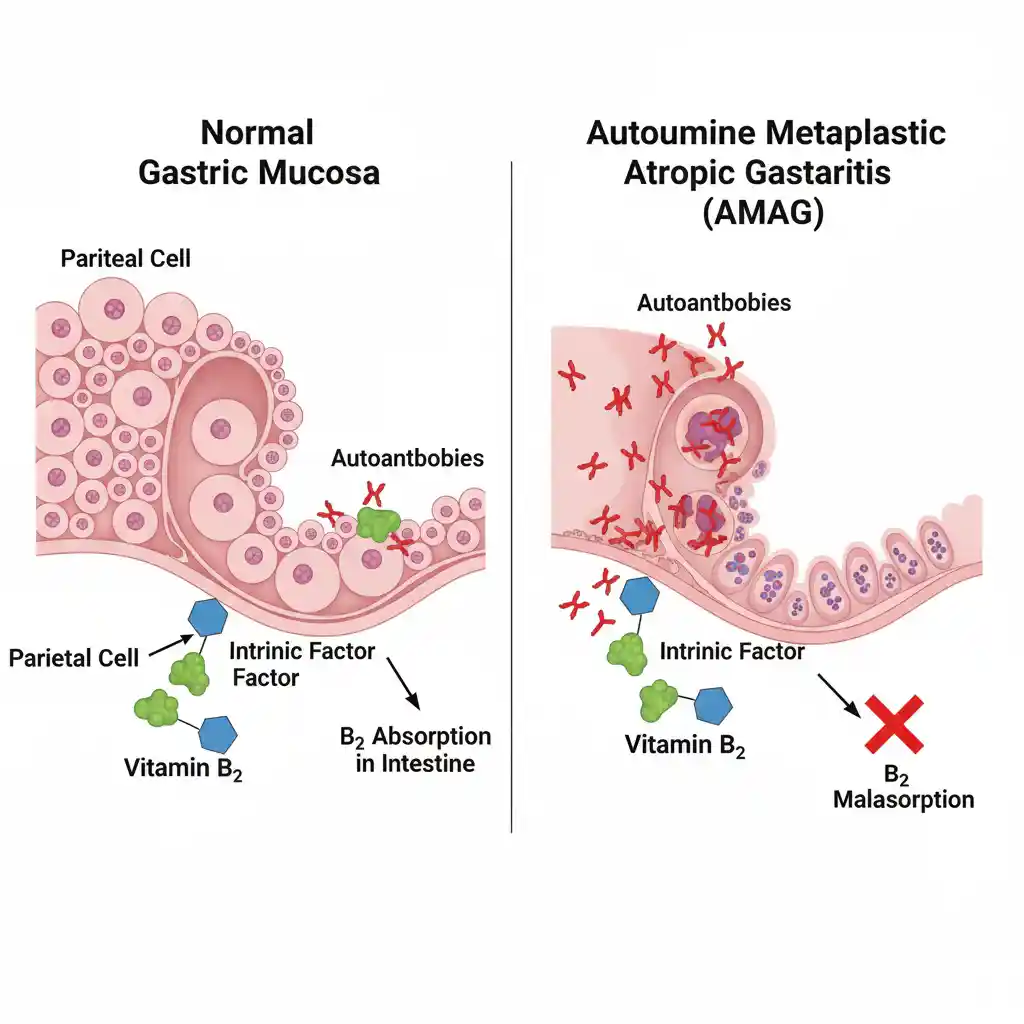
Atrophic Gastritis is a chronic histopathological entity characterized by the loss of native gastric glandular structures and their replacement by fibrosis or metaplastic epithelium (Intestinal Metaplasia). It represents a critical stage in Correa’s Cascade of gastric carcinogenesis. Etiologically, it is classified into Environmental Metaplastic Atrophic Gastritis (EMAG), primarily driven by Helicobacter pylori infection (Type B), and Autoimmune Metaplastic Atrophic Gastritis (AMAG), characterized by the destruction of parietal cells and subsequent Pernicious Anemia (Type A).
Clinical Coding & Classification
| System / Category | Code(s) | Description |
|---|---|---|
| ICD-10-CM | K29.40 | Chronic atrophic gastritis without bleeding |
| ICD-10-CM | D51.0 | Vitamin B12 deficiency anemia due to intrinsic factor deficiency (Pernicious Anemia) |
| CPT (Diagnostic) | 43239 | Esophagogastroduodenoscopy (EGD) with biopsy |
| CPT (Lab) | 83013 | Helicobacter pylori; breath test analysis |
| Staging System | OLGA / OLGIM | Operative Link on Gastritis Assessment (Histological Staging) |
Epidemiology & Statistics
The prevalence of atrophic gastritis correlates strongly with age and the endemicity of H. pylori. It is estimated to affect approximately 25% of the global population, with significantly higher rates in East Asia and South America. The condition confers a relative risk of 2.7 to 3.4 for the development of Gastric Adenocarcinoma compared to the general population.
Pathophysiology (Mechanism)
The progression involves distinct pathways based on etiology:
1. H. pylori-Associated (Type B): Persistent inflammation leads to the loss of glands in the antrum, spreading to the corpus. This induces Intestinal Metaplasia (replacement of gastric epithelium with intestinal-type cells), a precursor to dysplasia.
2. Autoimmune (Type A): Autoantibodies target the H+/K+ ATPase pump on Parietal Cells and Intrinsic Factor. This results in:
– Achlorhydria: Loss of acid secretion (elevated Serum Gastrin).
– Malabsorption: Vitamin B12 deficiency (Megaloblastic Anemia) and Iron deficiency.
Standard Management Protocols
Management focuses on halting progression to neoplasia and correcting nutritional deficits.
- Pharmacological Classes:
- H. pylori Eradication Therapy: (e.g., Bismuth Quadruple Therapy) Antibiotics + PPI. Essential to arrest mucosal atrophy progression.
- Vitamin B12 Supplementation: (e.g., Cyanocobalamin) Parenteral administration is required for Autoimmune Gastritis due to lack of Intrinsic Factor.
- Surveillance Protocols:
- High-Definition Endoscopy: Routine surveillance (every 3 years) is recommended for patients with extensive atrophy or intestinal metaplasia (OLGA Stage III/IV) to screen for early gastric cancer.
Healthcare Resource Utilization
Atrophic gastritis drives utilization of gastroenterology services:
- Endoscopic Surveillance: Repeat EGDs with mapping biopsies (Sydney System) consume significant resources but are vital for cancer prevention.
- Hematological Management: Long-term management of Pernicious Anemia.